The Digital Revolution in Mental Healthcare
Mental health affects millions globally. More than 264 million people worldwide live with depression. It is a major cause of disability, impacting lives and communities everywhere.
The past few years have highlighted this crisis more than ever. The COVID-19 pandemic acted as a major catalyst. It pushed us to rethink how we deliver mental health care, making innovation not just an option, but a necessity. Technology stepped in to fill critical gaps, offering new ways to connect and support those in need.
Today, we are in an exciting era of change. Innovations are changing mental health from every angle. From new treatments to better practice management, we see breakthroughs every day. These advancements promise a healthier future for everyone, whether through broad digital platforms or specialized care like that found at a mental health innovation Campbell County rehab.
We will explore the most significant advancements shaping our field. We will dig into how technology is changing service delivery and examine the ethical questions that arise. We will also look at how different countries approach innovation and what the future may hold. Join us as we find how these changes are improving patient outcomes and expanding access to vital mental health support.
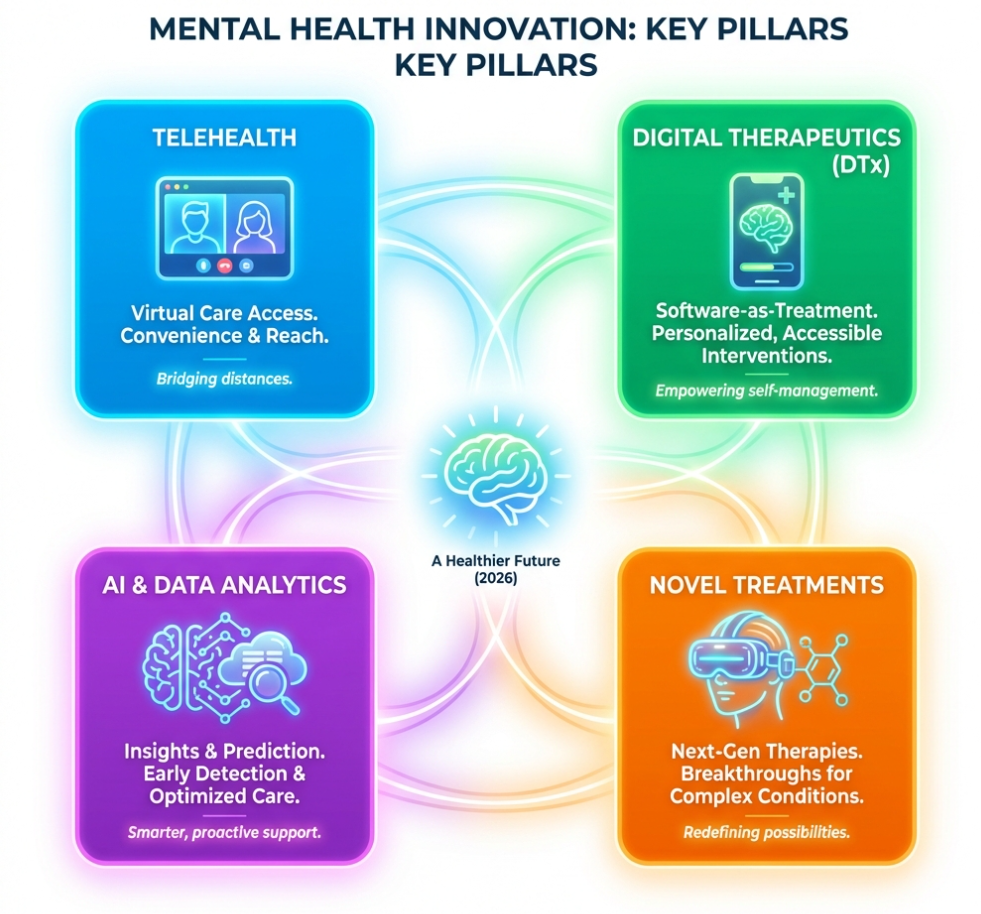
The landscape of mental healthcare has undergone a profound change, largely driven by digital advancements. What was once a niche offering, telehealth, has exploded into a mainstream method of care delivery. In 2014, telehealth clinical sessions represented a mere 0.15% of all healthcare services. The onset of the COVID-19 pandemic, however, dramatically accelerated its adoption. For instance, the Centre for Addiction and Mental Health (CAMH) in Canada witnessed an astonishing increase of over 850% in virtual care visits, soaring from approximately 350 per month to almost 3,000 between March and April 2020. Similarly, Kaiser Permanente, a major managed care organization in the United States, now delivers 90% of its psychiatric care virtually.
This rapid shift wasn’t limited to large institutions. A survey of 20 American psychiatrists revealed that all transitioned to fully virtual practices due to the pandemic, with most having no prior experience with telepsychiatry. The benefits of telepsychiatry and Internet-Delivered Cognitive Behavioral Therapy (iCBT) quickly became evident, offering convenience, reduced travel time, and increased access for many. Mental health apps also saw a surge in popularity. Platforms like Talkspace reported a 65% increase in clients since the pandemic began, demonstrating a clear demand for accessible digital solutions. Even specialized apps, such as PTSD Coach, have garnered significant attention with over 150,000 downloads, indicating a growing acceptance of digital tools in managing specific mental health conditions.
At the same time, traditional in-person services have started to blend with digital care, creating hybrid models that let patients move flexibly between face-to-face and online support. Many clinics now use video check-ins between full appointments, secure messaging for quick questions, and digital assessments that patients can complete before sessions. This creates a more continuous care experience rather than a series of isolated visits.

The Change of Therapeutic Access
The digital revolution has fundamentally altered how individuals access mental health support. One of the most significant benefits is the unparalleled convenience it offers. Patients can now receive care from the comfort of their homes, eliminating the need for travel and reducing time away from work or other responsibilities. This ease of access also plays a crucial role in reducing the stigma often associated with seeking mental health treatment. Engaging with a therapist or accessing resources digitally can feel less intimidating than traditional in-person appointments, encouraging more individuals to seek help.
Geographic accessibility has also dramatically improved. For those living in rural or underserved areas where mental health professionals are scarce, telehealth and digital platforms bridge critical gaps. Internet-delivered CBT, for example, has proven effective for anxiety and depression, with studies showing moderate to large effect sizes. This expansion of reach is vital, especially considering that an estimated 4 out of 5 people with mental disorders in low- and middle-income countries do not receive any form of mental health care. The growth of services like Talkspace further underscores the demand for flexible, remote options.
Beyond individual therapy, digital innovations are also fostering new community-based care models and localized support systems. These platforms can connect individuals with peers, support groups, and local resources, creating a more holistic network of care. Such advancements are being acceptd by forward-thinking facilities, with some dedicated recovery centers seeing it as a core part of their mission to provide comprehensive recovery support.
Digital tools are also changing the roles of families and caregivers. Secure portals can allow loved ones, with the patient’s consent, to receive updates, educational materials, and guidance on how best to support recovery at home. This shared approach can improve adherence to treatment plans and help identify early warning signs of relapse or crisis.
The Rise of Digital Therapeutics and Self-Help Tools
Beyond direct telehealth, digital therapeutics and self-help tools are emerging as powerful components of mental health innovation. These encompass a wide range of applications, from sophisticated mental health apps and AI-powered chatbots to immersive Virtual Reality (VR) experiences. VR, for instance, is showing promise in areas like cognitive and social rehabilitation, and even in improving symptoms of psychosis. These tools offer self-paced learning modules, allowing individuals to engage with therapeutic content at their own speed and on their own terms.
Gamification, the application of game-design elements and game principles in non-game contexts, is also being integrated into mental health apps to increase engagement and adherence. By making therapeutic exercises more interactive and rewarding, gamification can help overcome the challenge of low user retention often seen with mental health apps (where 96% of users may not engage after two weeks).
Common features found in top mental health apps include:
- Mood Tracking: Allowing users to log their emotional states and identify patterns.
- Guided Meditation and Mindfulness Exercises: Offering audio-guided sessions to promote relaxation and present-moment awareness.
- Journaling Prompts: Encouraging self-reflection and emotional processing.
- CBT Exercises: Providing structured activities to challenge negative thought patterns and develop coping skills.
- Goal Setting and Habit Building: Helping users establish healthy routines and work towards personal wellness objectives.
- Crisis Resources: Quick access to emergency contacts and helplines.
- Community Forums: Connecting users with peer support (often moderated).
- Educational Content: Articles, videos, and lessons on mental health topics.
More advanced digital therapeutics are being developed and tested like medications, with clinical trials, regulatory review, and defined indications (such as insomnia, substance use, or specific anxiety disorders). These tools can be prescribed by clinicians and often include dashboards that allow providers to see how patients are using the program between visits.
These digital tools represent a significant shift, empowering individuals with accessible, flexible, and often engaging ways to manage their mental well-being and access therapeutic support. When thoughtfully integrated with in-person care, they can extend the reach of clinicians, offer support between sessions, and give people practical strategies they can use any time, not just during an appointment.
Global Strategies and Successful Models in Mental Health Innovation
Mental health innovation is not confined to one region; it’s a global endeavor with various countries and organizations adopting diverse strategies to address their unique challenges. The United Kingdom, for example, stands out with its comprehensive approach to mental healthcare, particularly through its National Health Service (NHS). The UK’s mental health provision is pioneering a needs-led, outcome-focused, and responsive approach, prioritizing person-centered, compassionate, and supportive service delivery.
A landmark example is England’s Improving Access to Psychological Therapies (IAPT) program, launched in 2008. This program has transformed the treatment of adult anxiety disorders and depression, boasting an impressive over 50% recovery rate. Over a million people access IAPT services every year, highlighting its scale and impact. A key aspect of these global strategies is the emphasis on co-design with patients and the involvement of young people, ensuring that innovations are truly responsive to the needs of those they serve. Organizations like the Mental Health Innovation Network (MHIN) serve as vital hubs, connecting researchers, practitioners, policymakers, service user advocates, and donors worldwide to share innovative resources and ideas.

Patient and Community-Led Innovation
A crucial aspect of effective mental health innovation is the active involvement of patients and communities in the development process. This approach, often termed co-design, ensures that new solutions are not only clinically sound but also practical, acceptable, and relevant to the lived experiences of individuals. The “Youth Voice” movement, for instance, actively integrates young people into shaping mental health services and content that directly impacts them. This collaborative model empowers users, changing them from passive recipients of care into active partners in their own well-being.
The concept of “lived experience shaping research” is gaining significant traction, recognizing that insights from individuals who have steerd mental health challenges are invaluable. A prime example is Alder Hey Hospital’s Children and Young People (CYP) As One™ platform in the UK. This integrated mental health service platform was co-designed with over 100 children, young people, parents, and staff, ensuring it meets their real-world needs for referrals, support, and educational resources. Such initiatives demonstrate a commitment to creating user-centric solutions that are more likely to be adopted and sustained. For those interested in how these global networks foster collaboration, a valuable resource about the Mental Health Innovation Network’s Asia hub highlights regional efforts to advance mental health care.
Case Study: The UK’s Integrated Approach
The UK’s commitment to mental health innovation is further exemplified by its integrated approach, combining policy, research, and service delivery. The success of the IAPT program, with its high recovery rates for anxiety and depression, serves as a model for low-intensity mental health interventions globally. Furthermore, the National Institute for Health and Care Excellence (NICE) plays a pivotal role by providing guidance on health technologies. For example, NICE has released draft guidance recommending the conditional use of digital CBT for children with anxiety, demonstrating a proactive stance on integrating evidence-based digital solutions into care pathways.
The UK government has also made substantial investments in mental health research centers. The Mental Health Mission (MHM), launched in May 2023, represents a significant commitment, with £42.7 million invested to support innovation in research, services, and digital technology. This program aims to accelerate precision psychiatry and foster an alliance between people with mental health conditions and industry. Demonstrator sites, such as the Mental Health Research for Innovation Centre (M-RIC) in Liverpool and the Mental Health Mission Midlands Translational Centre (MHMTC), are revolutionizing mental health research by bringing patients and industry together to develop novel treatments for conditions like early intervention in psychosis, depression, and children’s mental health. For a deeper understanding of these strategic goals, a comprehensive resource about the UK’s Mental Health Goals provides further details on their ambitious plans.
Navigating the Problems: Ethics, Equity, and Scaling
While the promise of mental health innovation is immense, its implementation is not without significant challenges. Data privacy concerns top the list, especially with the proliferation of mental health apps. Many apps collect sensitive personal information, and their data sharing practices are often opaque. A study by Huckvale et al. (2019) found that many apps for depression and smoking cessation had concerning data sharing and privacy practices. This raises critical questions about who owns patient data, how it’s used, and whether it’s adequately protected.
User engagement is another hurdle. Despite the initial downloads, many mental health apps struggle with long-term retention. Baumel et al. (2019) found that 96% of users of popular mental health apps with over 100,000 downloads were not engaging with the app after just two weeks. This high drop-off rate indicates that simply developing an app isn’t enough; sustained engagement requires thoughtful design, personalized content, and often human support.
The “digital divide” poses a significant equity challenge. Access to reliable internet and digital devices is not universal. Tens of millions of North Americans, for instance, lack broadband access. This creates a barrier for low-income and rural populations who could benefit most from digital mental health solutions but lack the necessary infrastructure or digital literacy. Without addressing these fundamental inequities, digital innovation risks exacerbating existing disparities in mental healthcare access.
Ensuring Responsible and Ethical Innovation
To truly harness the benefits of mental health innovation, we must prioritize responsible and ethical development. This means embedding data security and patient confidentiality at every stage, adhering to regulations like HIPAA, and ensuring robust informed consent processes. The rapid pace of technological advancement often outstrips regulatory frameworks, creating a need for proactive measures.
The concept of “responsible innovation” provides a crucial framework. It emphasizes foresight, oversight, and societal deliberation to anticipate and mitigate potential harms while maximizing benefits. For example, Pinterest, a social media platform with around 335 million users, implemented a compassionate search experience. When users searched for terms indicating distress, they were directed to evidence-based cognitive behavioral practices, with all interactions kept private and anonymous, and no tracking data collected. This demonstrates how technology can be used responsibly to support mental well-being without compromising user privacy.
Such examples highlight the importance of designing technology with ethical considerations from the outset. For a deeper dive into the principles and practices necessary for navigating these complex issues, a valuable resource about responsible innovation in technology for mental health offers detailed insights.
Overcoming Barriers to Widespread Adoption
Scaling successful mental health innovations to reach a wider population presents several complex challenges. One significant barrier is cost-effectiveness. While digital solutions can reduce some costs, the initial investment in development, infrastructure, and training can be substantial. Demonstrating long-term cost savings and improved outcomes is crucial for widespread adoption by healthcare systems and insurers.
Regulatory problems also slow down progress. New digital therapeutics often don’t fit neatly into existing regulatory categories, leading to delays in approval and reimbursement. Clearer, more agile regulatory pathways are needed to bring effective innovations to market faster. Training healthcare providers to effectively integrate new digital tools into their clinical workflows is another critical component. Many practitioners, particularly those who are not digital natives, require comprehensive training and ongoing support to feel confident and competent using these technologies.
Finally, addressing inequities in access remains paramount. This involves tackling the digital divide by expanding broadband infrastructure and providing affordable devices, as well as addressing digital literacy gaps through education and support programs. Hospitals and clinics could offer “digital rooms” for patients without home access, and governments could provide free smartphones to those who cannot afford them. Without these concerted efforts, even the most groundbreaking innovations will fail to reach those who need them most.
The Future Horizon: AI, Policy, and Personalized Care
The future of mental health innovation is ready for even more transformative changes, with Artificial Intelligence (AI) and advanced data analytics at the forefront. Predictive analytics, driven by big data, are shifting mental health research from a reactive to a proactive stance. By analyzing vast datasets, including social media data, researchers can identify early warning signs of mental health deterioration and predict trends across populations. This allows for more timely interventions and targeted resource allocation.
Novel drug therapies are also on the horizon. Beyond traditional antidepressants, new compounds are being explored that target different neurochemical pathways, offering hope for treatment-resistant conditions. For instance, esketamine has been approved for treatment-resistant depression, representing a significant step forward. Furthermore, research into psychedelics like psilocybin and MDMA for conditions such as major depressive disorder (MDD) and PTSD is showing remarkable promise, potentially offering transformative treatments for individuals who have not responded to conventional therapies. These advancements, coupled with the increasing role of big data, are paving the way for a new era of personalized and highly effective mental healthcare.
Feature Traditional Diagnostics AI-Driven Diagnostics Data Source Patient self-report, clinical observation Wearable data, smartphone usage, social media, EHRs Speed Slower, reliant on appointments Real-time, continuous monitoring Personalization Limited, based on broad categories Highly personalized, adaptive to individual patterns Predictive Power Reactive, focused on current symptoms Proactive, identifies risk factors and early warnings The Role of AI in the future of mental health innovation
Artificial Intelligence is set to revolutionize mental health care by enabling unprecedented levels of early detection, personalized interventions, and efficient service delivery. AI algorithms can analyze passive data collected from smartphones, wearables, and other digital interactions to identify subtle changes in behavior, sleep patterns, or communication styles that may signal an impending mental health crisis or relapse. This capability moves us closer to preventative mental healthcare, allowing for interventions before conditions escalate.
AI can also power highly personalized interventions. Chatbots, for example, can deliver custom therapeutic content and support, adapting to a user’s specific needs and progress. Natural Language Processing (NLP), a subfield of AI, is being used to analyze text and speech patterns in therapy sessions, providing therapists with insights into treatment effectiveness and patient engagement. For practitioners, AI-powered mental health innovation is streamlining administrative tasks, automating routine processes, and providing deeper insights into therapy sessions, freeing up clinicians to focus more on direct patient care. This integration of AI promises to improve both the efficiency and effectiveness of mental health services.
Supporting the next wave of mental health innovation
Sustaining the momentum of mental health innovation requires robust policy frameworks and consistent funding. Governments worldwide are recognizing the urgency and are beginning to invest significantly. This includes direct funding for research and development, as well as creating incentives for public-private partnerships. These collaborations are crucial for translating scientific findies into scalable, real-world solutions.
However, investment alone is not enough. The field needs robust evaluation frameworks to rigorously assess the effectiveness, safety, and ethical implications of new technologies and treatments. Without clear evidence of efficacy and cost-effectiveness, widespread adoption will remain challenging. Policymakers must work to streamline regulatory processes while ensuring patient safety and data privacy. Furthermore, initiatives that build research capacity and foster international collaboration are vital. For example, the National Institute of Mental Health (NIMH) supports research on digital mental health technologies, emphasizing development, testing, implementation, and cost-effectiveness across diverse populations. A valuable resource about the NIH’s Digital Global Mental Health Program outlines their commitment to advancing this critical field. By focusing on these pillars, we can ensure that the next wave of mental health innovation is both groundbreaking and responsibly implemented.
Frequently Asked Questions about Mental Health Innovation
What are the most significant innovations in mental health today?
The most significant innovations currently changing mental health care include the widespread adoption of telehealth and telepsychiatry, making services more accessible than ever before. We’re also seeing rapid advancements in AI-driven diagnostics and support tools, such as intelligent chatbots and predictive analytics for early detection. Digital therapeutics, including prescription apps that deliver evidence-based interventions, are gaining traction. Furthermore, novel treatments like esketamine for treatment-resistant depression and groundbreaking research into the therapeutic potential of psychedelics (psilocybin, MDMA) are offering new hope for complex conditions.
How is technology changing mental health services?
Technology is fundamentally reshaping mental health services by increasing accessibility, personalization, and continuity of care. Virtual appointments via telehealth overcome geographical barriers and reduce stigma, allowing more people to connect with therapists. Digital platforms and apps provide continuous support through features like mood tracking, guided meditations, and CBT exercises, empowering individuals in their self-management. AI and data analytics enable more personalized treatment plans and the early detection of mental health issues, while also streamlining administrative tasks for practitioners. This digital shift fosters a more flexible, responsive, and patient-centric model of care.
What are the main challenges facing mental health innovation?
Despite the progress, several key challenges persist. Ensuring patient data privacy and security is paramount, as digital platforms handle highly sensitive information. Overcoming low user engagement and high drop-off rates for many digital tools is crucial for long-term effectiveness. Addressing the digital divide, which includes unequal access to broadband internet and devices, is essential to ensure equitable access to innovations. Finally, developing clear and agile regulatory pathways for rapidly evolving digital technologies, along with training healthcare providers to effectively integrate these new tools, remains a significant hurdle.
Conclusion: Embracing a New Era of Mental Wellness
The journey through the landscape of mental health innovation reveals a field brimming with transformative potential. From the explosive growth of telehealth and the increasing sophistication of digital therapeutics to the groundbreaking insights offered by AI and novel pharmacological treatments, we are truly entering a new era of mental wellness. These innovations are dismantling traditional barriers to care, offering unprecedented accessibility, personalization, and support to millions worldwide.
However, as we accept these advancements, it is crucial to maintain a balanced and thoughtful approach. The ethical considerations surrounding data privacy, the imperative for equitable access, and the challenges of scaling successful interventions demand our continuous attention. Responsible innovation, guided by robust research and a deep understanding of lived experience, must be at the core of our efforts.
The future of mental health is a collaborative endeavor. It requires sustained investment from governments, agile policy development, and strong partnerships between researchers, clinicians, technologists, and, most importantly, individuals with lived experience. By working together, emphasizing responsible, equitable, and evidence-based implementation, we can ensure that the promise of mental health innovation translates into a healthier, more supportive future for everyone. Let us seize this moment to build a mental healthcare system that is truly responsive, resilient, and ready for the challenges of tomorrow.
Meta Title: Mental Health Innovation: Unlocking 2026’s Future
Content Slug: innovations-in-mental-health-from-treatment-to-practice-management
Meta Description: Explore cutting-edge mental health innovation: telehealth, AI, and digital tools. Discover how technology transforms care access and outcomes.